
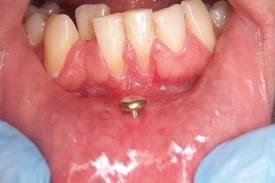

This four-part article series covers the many habits - some innocent, some not-so innocent - that could be destroying your teeth and oral health, leading to the need for dental implants. Welcome back to our four-part article series in which New Teeth in NJ specialists explain the top habits and behaviors that could be wrecking the health of your teeth and gums. In our previous article post, the first of the series, chewing ice and playing sports without a mouth guard were discussed as the first two harmful habits. We’ve got many more to get through - some you may already be aware of but others that may come as a surprise - so let’s get straight back into it! Teeth-Wrecking Habit # 3: Giving Baby a Bedtime Bottle  Handing your tiny tot a bottle as they go to bed may help them fall asleep, but it could also lead to early tooth decay! Whether it’s formula or juice, both contain sugar and bacteria love sugar. Giving your child a bottle to suck overnight leaves their developing teeth and gums in a veritable sugar bath, which is oral bacteria’s idea of paradise. Feed your baby before you put him or her to bed and be sure to gently clean their mouths afterwards. If they want something to suck on, give them water or a pacifier. ‘The development of a child’s adult teeth can be severely impacted by the health of their predecessors, the baby milk teeth,” explain New Teeth or dental implant specialists. “As such, it’s imperative that parents take the correct actions in looking after their children’s pearly whites. Also note that you should throw the pacifier in the trash bin after age 1. Constant sucking on these kinds of appliances can actually change the shape of the mouth and can result in severe orthodontic problems.” Teeth-Wrecking Habit # 4: Lip and Tongue Piercings  Feeling rebellious? Try a tattoo... lip and tongue piercings can do serious damage to your dental enamel! Accidentally biting down on the stainless steel bar or the constant tapping of the piercing against the back of your teeth as you talk can cause chipping and cracks. In the case of lip piercings, the metal disk on the inside of the lip can rub against the gums causing irritation, inflammation and even infection. The gums can become so damaged that they actually recede from the crowns of the teeth, revealing the darker root underneath (see image above). Tongue piercings can also make it difficult for you to clean your tongue properly. This is not even to mention the risk of infection such invasive activities cause. Again, if you’re feeling rebellious, do something really brave like get a tattoo or dye your hair shocking pink, instead. Leave your mouth alone! Teeth-Wrecking Habit # 5: Tobacco-Use  Perhaps the least surprising of all the bad habits on this list are smoking and tobacco-use. We won’t bore you with the details, but in short, tobacco-use: • Stains the teeth, • Causes dry mouth, • Causes bad breath: “smoker’s halitosis”, • Irritates and inflames (burns) the soft tissues in the mouth, • Slows the natural healing process, • Renders various procedures less likely to succeed, such as dental implants, • Increases your risk of developing oral cancer, • Causes gum infection and disease. Stay Tuned for Part 3 If you like your current pearly whites and want to avoid needing new teeth later on in life, stay tuned for the third installment of this four-part article series to find out more of the bad habits, behaviors and addictions you should be avoiding!
1 Comment
Dental Implants Specialists In Rutherford Talk About The Habits That Ruin Your Teeth, PART 15/9/2013 This four-part article series covers the many habits - some innocent, some not-so innocent - that could be destroying your teeth and oral health, leading to the need for dental implants. Sharks have multiple sets of teeth. In fact, they tend to grow a fresh set of teeth every two weeks or so to replace those ripped out during feeding frenzies. Rodents have incisors that just keep growing and growing, which is why - in part - beavers gnaw incessantly on the boles of trees: to prevent their teeth from getting too long. Elephants have a set of molars that steadily march towards the front of their mouth during the course of their lifetime. At age 40, a set of larger brand new molars emerge to replace those that have been ground down by day-long munching. But, humans have only two sets of teeth. The first start to emerge soon after we are born and are then replaced with adult teeth in our late childhood.  In other words, by the time we are 12, we have the set of teeth that is meant to last us for the rest of our lives. There are no second chances for us. Unlike sharks, we won’t sprout new teeth to replace those lost through bad oral hygiene or an accident. Our teeth, if chipped, won’t keep growing and at age 40 we’re more likely to lose our molars than grow a fresh set like elephants! This is why it’s so important that we look after our pearly whites from as early an age as possible. In this four-part article series, dental implants specialists in Rutherford - the dental healthcare professionals responsible for replacing missing teeth – will be taking us through their top list of habits and behaviors that are ruining the health of your teeth and gums and could possibly lead to early tooth loss. Some of these habits you may be aware of already, such as smoking, but others will come as a surprise! So, without further ado, let’s get started... Teeth-Wrecking Habit # 1: Chewing Ice  On a hot day, it can be wonderful to fill a cup with ice and soda and sit there chewing on the lumps and shards of ice. While ice is sugar-free and, in its liquid state, is perfectly good for you, your teeth were not made to bite into it! In a battle between enamel and ice, enamel is likely to win, but that doesn’t mean it will win every time and the result could be fractures, cracking and chipping. Also, if you make it a habit you could end up irritating the soft tissues inside your teeth, or even grind the enamel down to the dentine, leaving your pearly whites far more vulnerable to cavities and decay. “If you’re a compulsive chewer, buy yourself some sugar-free gum,” suggests a specialist of dental implants in Rutherford. “Chewing ice is terrible for the enamel of your teeth and if you don’t address it, I will expect to see you in my office before long.” Teeth-Wrecking Habit # 2: Playing Sports without a Mouth Guard  Think twice before getting on the field or ring without a mouth guard! It just takes one second for something to go horribly wrong and for teeth to go flying. You wouldn’t stand in front of the ice hockey goal without the correct protection - you could literally get yourself killed should the puck fly at your face at just the right angle - so why would you face the football player without a helmet and mouth guard? In fact, most sports (other than badminton… but who plays badminton?) come with a risk of facial trauma. “Make sure you invest in a good mouth guard and wear it,” advises the dental implants specialist in Rutherford. “If your friends laugh at you, tell them to Google mouth sports injuries… that’ll zip their lips.” Stay Tuned for Part 2 If you like your current pearly whites and want to avoid needing new teeth later on in life, stay tuned for the second installment of this four-part article series to find out more of the bad habits and behaviors you should be avoiding! This four-part article series explains the meaning to some rudimentary dental implant terminology that patients might come across on their journey to getting new teeth. Welcome back to our four-part article series on some rudimentary terminology you might like to know if you’re thinking of having new teeth implants placed. In our previous article installment, the third part of the series, we reviewed some important terms pertaining to full mouth reconstruction, including bone grafting, which is a procedure that is done to augment and encourage the growth of new and healthy bone tissue in the jaw so that dental implants can be placed. We also provided a brief description of the All-on-4 dental implant protocol and osseointegration, the process whereby bone tissue forms a strong biological bond with the titanium surface of an implant. In this article, the final installment of our four-part series, we’ll provide a brief explanation of tooth anatomy before discussing the various oral conditions that cause tooth loss and Cone Beam Computed Tomography, an indispensible diagnostic tool used by the oral specialists that offer patients new teeth with dental implants. Dental Terminology You Might Like to Know! 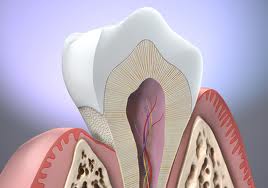 The Anatomy of a Tooth: Your teeth consist of a hard outer coating of dental enamel, which protects the delicate insides from infection and contamination by bacteria. Beneath the enamel is a slightly softer and more porous substance called dentin. Within the heart of the tooth resides the pulp chamber, within which lie all the tooth’s nerves and blood vessels (called the pulp). This chamber narrows at the base of the tooth into the thin canals that run the length of the roots (root canals). Cone Beam Computed Tomography (CT): CBCT is a diagnostic imaging tool that emits a cone-shaped beam of X-ray radiation. The resultant images are translated into digital data by the machine and this is fed into a computer software program. The oral specialists who use CBCT can use this software to view a highly detailed and accurate 3-D picture of their patient’s dentition, tooth orientation and jawbone structure (see image below). This, in turn, enables them to plan dental implant surgery before the patient has even come in for the procedure. By determining the best possible sites for dental implant placement prior to surgery, oral surgeons can reduce risks, complications and the chance of implant failure. Cone Beam CT also decreases the degree of invasiveness, thus decreasing recovery time and patient discomfort. 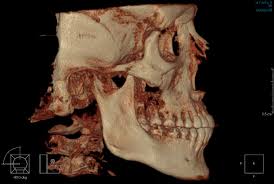 Periodontal (Gum) Disease: An advanced oral bacterial infection of the gums surrounding the teeth. Periodontal disease, or periodontitis, is the advanced stage of gingivitis and is marked by gum inflammation and recession, chronic bad breath, oral lesions, tooth discoloration and tooth loss. Periodontal disease is the number one cause of tooth loss in the United States. Risk factors for this condition include smoking, heavy drinking, poor oral hygiene and illnesses such as diabetes, osteoporosis and rheumatoid arthritis. Edentulism: The state of not having a single original adult tooth left. There are currently an estimated 38 million edentulous people living in the United States. These people desperately need new teeth, yet instead of opting for a sophisticated teeth replacement solution like the All-on-4, they instead tend to wear removable dentures. Plaque: A whitish sticky substance that can be scraped off the teeth with a fingernail. Under the microscope, plaque is revealed to be millions upon millions of bacterium. There are over 700 different kinds of bacteria in plaque! Tartar: Hardened deposits of plaque, which offer bacteria an excellent hiding place away from the roving bristles of your toothbrush. Tartar causes tooth decay and tooth loss... and it can only be removed by a dental healthcare professional, which is why it’s so important to visit your oral hygienist twice a year! This four-part article series explains the meaning of some rudimentary dental implant terminology that patients might come across on their journey to getting new teeth. Welcome back to our four-part article series on the rudimentary terminology you might like to know if you are looking into getting new teeth in one day. In our previous article installment, part two of the series, we provided definitions for two conventional teeth replacement technologies: non-implant supported bridges and removable dentures. We then went on to explain the dangers often associated with these technologies, which only replace the visible portion of missing teeth - alveolar atrophy. Let’s now take a look at bone grafting and a sophisticated dental implant procedure that can be used to give patients presenting with advanced jaw bone loss new teeth in as little as a single day! Dental Terminology You Might Like to Know! 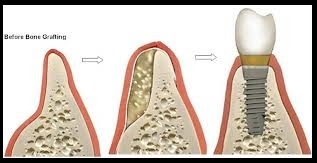 Bone Grafting: “Bone grafting” is procedure whereby bone tissue is acquired from another part of the body (or another source) and used to augment the jaw in site/s of depleted bone volume. As it was discussed in Part 2 of this article series, bone loss is generally a result of tooth loss and alveolar atrophy. In the context of oral and maxillofacial surgery, bone grafting is done to augment and encourage the growth of new and healthy bone tissue in the jaw so that dental implants can be placed. Bone grafting is an invasive procedure and is therefore can be quite traumatic and painful for patients to go through. It is also expensive and usually requires many months of healing before the jawbone is strong enough to accept implants. The “All-on-4": The All-on-4 is a revolutionary dental implant technique that was first introduced to the market in the early 1990’s. Since it’s innovation by European implantologist, Dr. Paulo Malo, it has enjoyed tremendous success worldwide due to its ability to provide patients suffering with failing dentition (or who have lost most if not all of their original adult teeth) with a brand new set of fixed teeth in as little as a single day, with a single surgery. This treatment time goes without precedent: Traditional dental implant procedures and techniques could require as many as 18 months to give patients new teeth. 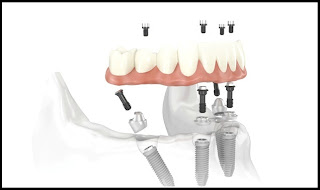 This All-on-4 protocol consists of the strategic placement and angulation of four dental implants in regions of the jawbone that are more resistant to the atrophy caused by tooth loss (see image above). Through the careful planning of implant sites, oral specialists are almost always able to find enough support for a customized, non-removable (fixed) prosthetic dental bridge, without the need for bone grafting first. This saves patients in need of new teeth the trauma and expense of undergoing such a procedure, while also saving them the many months that would otherwise be spent in recovery. For these reasons and many more, the All-on-4 is considered a “breakthrough” in the fields of dental implantology and fixed oral rehabilitation. Osseointegration: The process whereby bone tissue biologically bonds or fuses with the surface of an implant. Titanium is completely biocompatible, so the body typically does not reject the implant. Rather, the bone cells attach themselves to its surface and new bone grows around the implant. 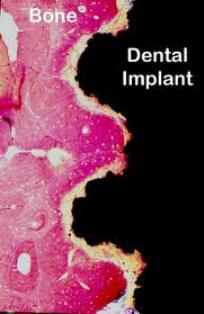 Stay Tuned for Part 4 To learn more about dental implants and oral health terminology, stay tuned for the final installment of this four-part article series. This four-part article series explains the meaning to some rudimentary dental implant terminology that patients might come across on their journey to getting new teeth. Welcome back to our four-part article series on some rudimentary terminology you might like to know if you’re in need of new teeth in one day! In our previous article installment, the first of the series, we opened with a look at some of the most important concepts to become familiar with: Dental implants are tiny titanium screws that are placed in the jawbone and are used to support a replacement tooth, which can either be a dental crown (in the case of a single tooth replacement) or a fixed bridge (as in the case of full arch restoration). An abutment or “collar” is the component that attaches the visible replacement tooth to the dental implant. Let’s continue with a definition of some of the older, more conventional teeth replacement technologies that are still available today... Dental Terminology You Might Like to Know! 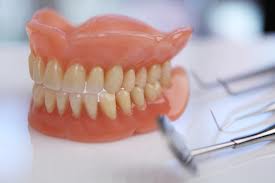 Removable Dentures: Removable dentures (see image above), commonly known as “false teeth”, are the conventional teeth replacement option for patients who are in need of new teeth. They resemble a complete set of teeth and gums, but are far bulkier than fixed bridges because they rely on their mass and the support of the gums and oral structures to keep them stabilized in the mouth. Without anything “permanent” holding dentures in place - like dental implants - removable dentures are free to move around and, in extreme cases, can even fall out. They can often be uncomfortable and insecure, as well as needing to be removed for cleaning and at nighttime. Removable dentures only replace the visible portion of the missing teeth, the crowns, and not the roots. This facilitates the bone that formerly surrounded the tooth roots to atrophy and waste away (see atrophy below). Non-Implant Supported Dental Bridge: The conventional approach to replacing one or two adjacent missing teeth is to file down the neighboring healthy teeth and use them to support a “bridge” or linked series of replacement dental crowns as is shown in the picture below. 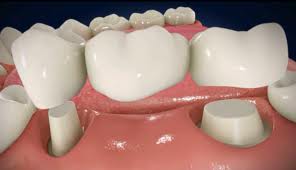 The two adjacent teeth are “prepared” in order to support the middle crown, which is one of the reasons dental implants are considered a more advantageous solution to missing teeth (they don’t require the involvement of adjacent healthy teeth). While non-implant supported crowns offer aesthetic solutions, they do not replace the root of the missing tooth and, similarly to removable dentures, this can lead to atrophy of the underlying jawbone. Alveolar Atrophy: The alveolus is the part of the jawbone that houses the teeth. When teeth are lost, this bone typically disappears as it becomes resorbed by the jaw. Similar to the muscles in your body, bone tissue requires stimulation or “exercise” to stay healthy. The tooth roots are responsible for keeping the jawbone stimulated and they do this by transmitting the forces associated with eating (grinding, chewing and incising) into the underlying bone tissue. When the roots of the teeth are lost, so too is this stimulation and as a result, the bone that formerly encased the tooth roots (the alveolus) atrophies and disappears. The result of bone loss has a widespread impact upon one’s oral health: it often upsets the stability of the neighboring teeth and can even cause further tooth loss. Bone loss also puts a patient’s candidacy for dental implants in jeopardy, because implants, just like natural teeth, require adequate bone volume in order to remain rooted in the jaw. 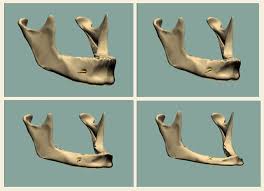 Replacing missing teeth with conventional technologies, such as traditional bridges and removable dentures, is ineffective in preventing alveolar atrophy because they only replace the visible tooth structure and not the roots. This is why dentures need replacing every few years or so - because they fail to fit the changing shape of the jawbone. This is also why dental healthcare specialists recommend dental implants to patients in need of new teeth. Stay Tuned for Part 3 To learn more about dental implants and oral health terminology, stay tuned for the third installment of this four-part article series. This four-part article series explains the meaning to some rudimentary dental implant terminology that patients might come across on their journey to getting new teeth. Do you need one or more of your teeth replaced? According to statistics released by the American Dental Association, tooth loss would seem to be an inevitable part of life. Even if you care for your teeth properly and seek regular professional attention from a dental healthcare expert, chances are you’ll lose at least one of your teeth during the course of your lifetime. When you do lose a tooth, it is imperative that you seek out the best possible tooth replacement option available so that you can continue your day-to-day as comfortable and confident as possible! What is the best option? Dental implants, of course! So, if you need new teeth, here is some terminology you might like to know before you hit the specialists’ office. Dental Implant Technology  Dental Implant: A freestanding artificial tooth root constructed from medical grade titanium metal. This tiny screw is inserted at the site/s of the missing tooth or teeth, or at pre-determined locations in the jawbone and is usually used to support either a ceramic tooth crown (in the case of single tooth replacement) or a prosthetic dental bridge (as in the case of full arch reconstruction). Dental Crown: A dental crown is typically a ceramic restoration that is used to replace large portions of the natural tooth structure that have had to be removed due to physical injury or decay. When supported by a dental implant, crowns can be used to replace the entire tooth structure visible above the gum line. They are carefully shaped to closely resemble natural teeth and are made of strong and durable materials that mimic the optical properties of dental enamel. If you have lost one or two of your teeth, you will most likely have implant-supported crowns placed. The image above clearly shows the titanium dental implant, which serves as the “anchoring root” for an artificial tooth crown. Usually, the only visible component of this tooth replacement technology is the durable ceramic crown and this is fabricated to be virtually indistinguishable from any of the neighboring natural teeth. Abutment or “Collar”: The abutment is the component that connects the ceramic crown (replacement tooth) to the dental implant, which resides below the gum line. Together, the implant, abutment and crown make up an entire replacement tooth. 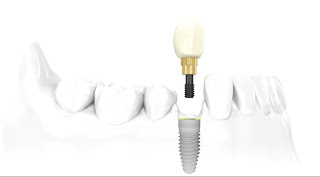 Bridge (Fixed): A fixed bridge is essentially a complete set of artificial teeth and gums, usually made from a durable metal framework along acrylic or ceramic teeth, which is held permanently in place using dental implants in NJ. A bridge is carefully fabricated to closely resemble a full set of natural teeth and gums and is an excellent solution for patients who have lost most or all of their original adult teeth or who suffer from a failing dentition. Owing to the durability of the materials from which it is made, a fixed bridge can also support a strong and natural bite, enabling patients to eat most foods. Stay Tuned for Part 2 To learn more about dental implants and oral health terminology, stay tuned for the second installment of this four-part article series. This article provides an over-view of periodontal (gum) disease: what it is, how it develops, what the symptoms of it are and how patients can prevent it. Periodontitis or periodontal disease and gum disease are one and the same thing: one of the greatest causes of tooth loss in the United States. Left untreated, this terrible oral affliction is, more so than any other oral offender, guilty of leaving people without a single original adult tooth in their mouths. Sounds shocking, doesn’t it? Well, it shouldn’t be because currently 30% of our population is completely edentulous (toothless) and in dire need of new teeth as a result of gum disease! It’s a prevalent condition and is remarkably easy to develop, given the right mix of oral hygiene negligence and bad lifestyle. In order to increase awareness of the dangers of periodontitis, we shall be exploring what this disease is, what the symptoms of it are and how you can go about preventing it from laying waste to your beautiful, youthful smile. What is Periodontitis? 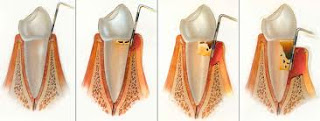 Periodontitis or gum disease is an advanced oral bacterial infection of the gums surrounding the teeth. In its early stages, such a condition is referred to as “gingivitis”. If allowed to progress without treatment or intervention of any kind, this infection can become advanced and migrate deep down into the gingival sulci or tooth sockets (see image above). Here, safe from the roaming bristles of your toothbrush or any other hygienic measure, the bacteria are left allowed to proliferate. Before long, deep pockets of bacterial waste and other nasty toxins accumulate between the gum walls and the roots of the teeth causing tooth decay and ultimately, tooth loss. What are the Signs and Symptoms of Periodontitis? 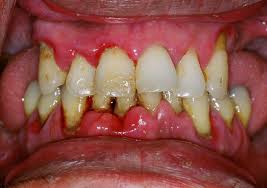 In the initial stages of the disease, when it’s still known as “gingivitis” you may notice: • Red, inflamed gums, • Swollen gums that form larger “bubbles” between the teeth, • Gums that tear and bleed easily, especially when brushing and flossing, • Chronic bad breath, • Some tooth discoloration caused by visible accumulations of calculus on the teeth. In the advanced stages of gum disease, you may notice any or all of the above-mentioned symptoms in addition to: • Gums that have receded unnaturally from the crowns of the teeth, exposing the darker roots underneath and leaving you looking “toothy”, • Tooth discoloration, • A brown mottling between the teeth and at the gum margins, • Oral lesions or sores, • Loose teeth, • Teeth that fall out. How Can I Prevent Gum Disease?  Periodontitis is caused by oral bacteria, which is thankfully easy to keep under control with good oral hygiene and regularly scheduled appointments with the dentist and oral hygienist. Avoiding tooth loss and the need for new teeth also come down to certain lifestyle choices, such as staying away from: • Smoking • Heavy drinking • Drug abuse • Eating disorders • An unhealthy diet high in sugar and starch. If you manage your health and any illnesses you may have (such as diabetes) and if you look after your teeth and gums, you should be able to keep them in excellent condition for life. Any implant specialist will tell you that not even dental implants can rival the sophistication and longevity of your own biological technology! |